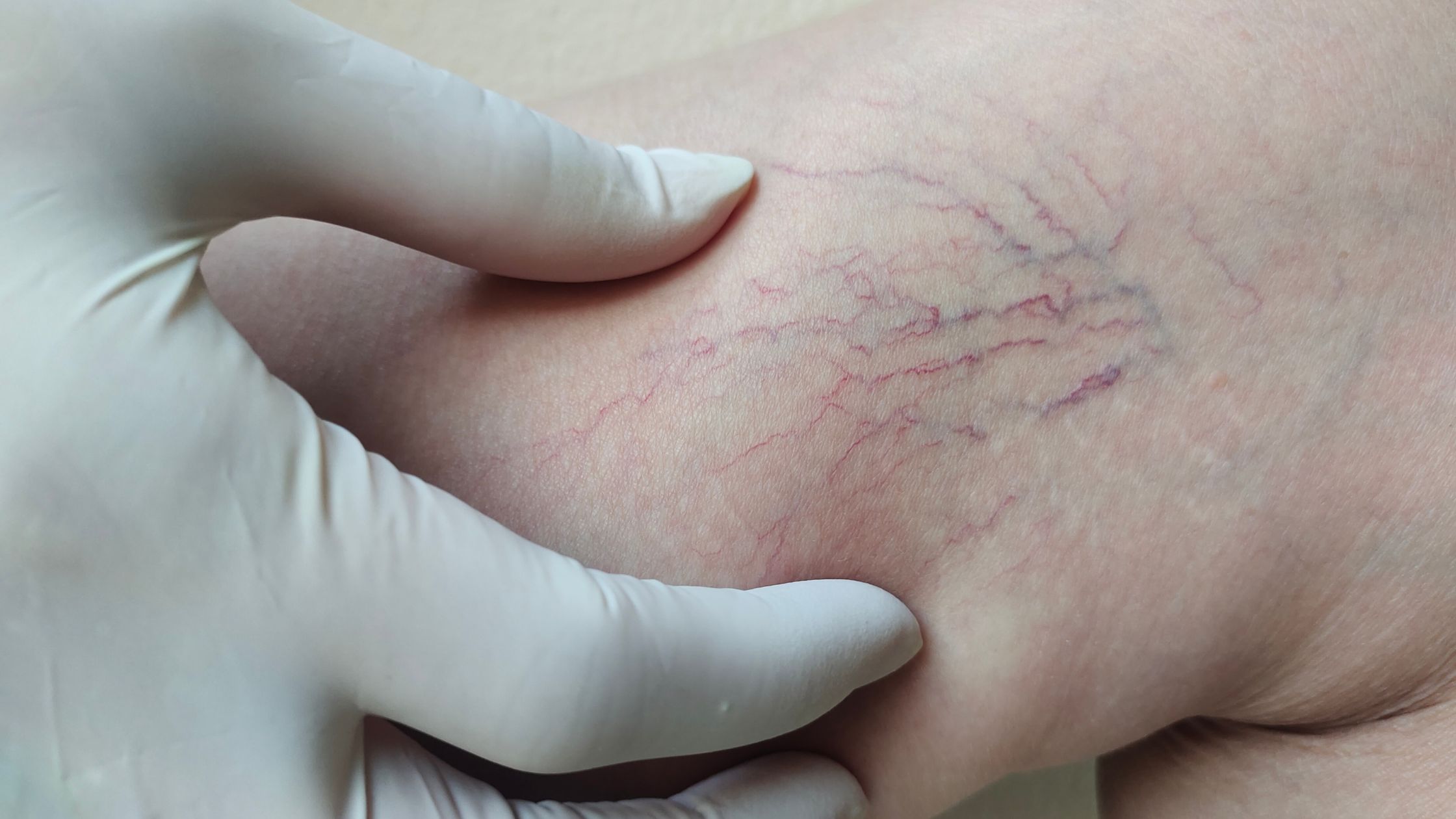
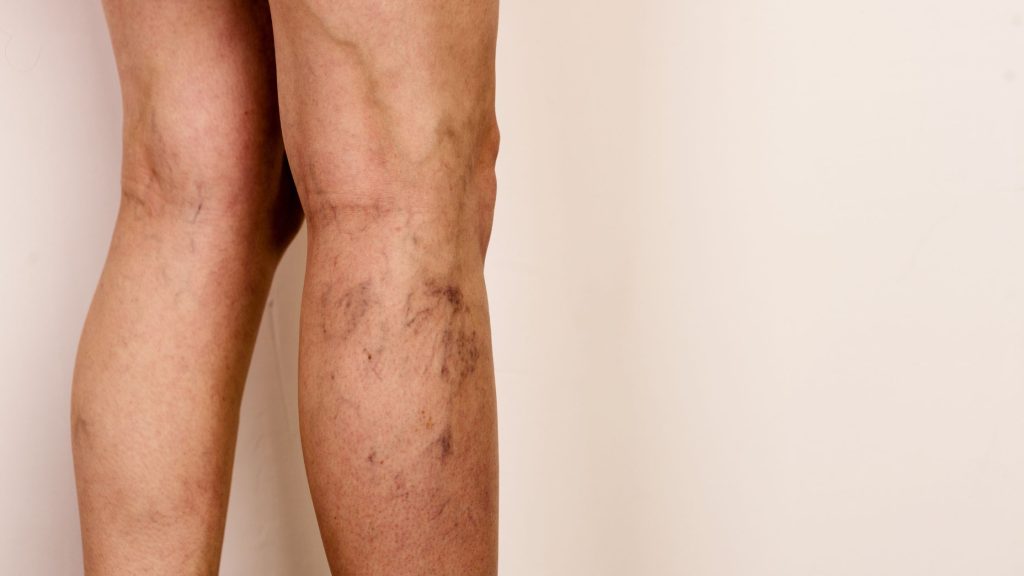
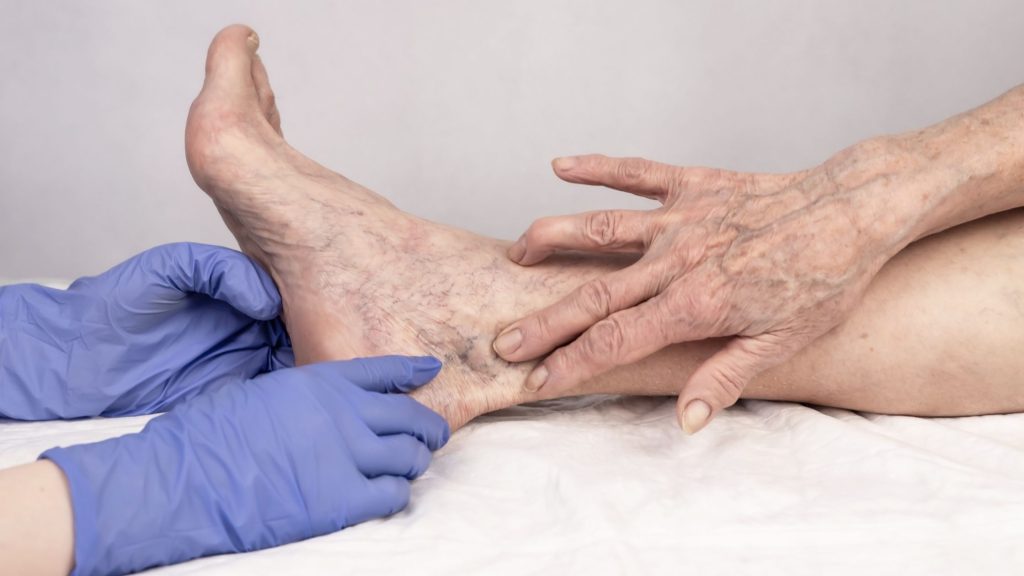
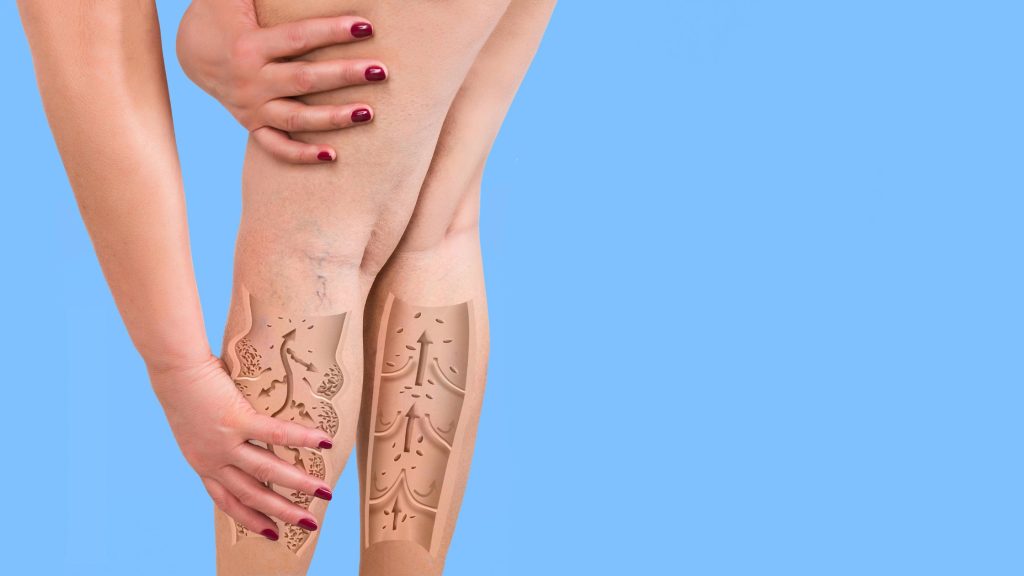
For many, discovering spider veins on the ankles or face is often dismissed as a purely cosmetic nuisance. However, these small, jagged lines can sometimes be the first outward signal of deeper vascular health issues.
While they are generally less severe than bulging varicose veins, understanding what causes spider veins and knowing when to worry about the condition is crucial for long-term circulatory health.
In this guide, we explore the early signs of venous insufficiency and why consulting a specialist like a board-certified cardiologist can make all the difference in your treatment journey.
Understanding Spider Veins
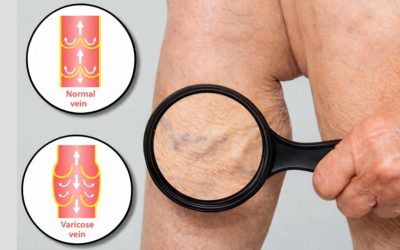
A spider vein (telangiectasia) consists of small, dilated, damaged blood vessels that appear near the surface of the skin. They develop when tiny capillaries in the dermis (middle layer of skin) become enlarged and overfilled with blood. Moreover, they often resemble thin spider webs or tree branches and typically appear in shades of red, blue, or purple.
Unlike deeper veins that pump blood back to the heart, these superficial vessels function primarily for temperature regulation. When they weaken or dilate, blood pools, making them appear as visible red, purple, or blue lines—often resembling a spider web or tree branches.
According to vascular dermatology research, spider veins affect approximately 30-60% of the population at some point in their lives, making them one of the most common vascular conditions. In fact, women are more likely to develop them than men.
While common on the legs, many patients also seek help for a facial spider vein or a spider veins on nose concern, which can be triggered by sun exposure or pressure.
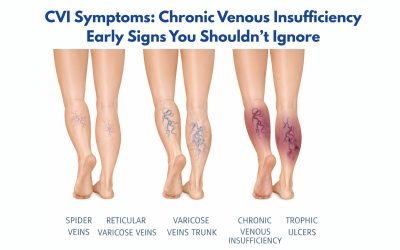
Early Signs of Spider Veins
Identifying the condition early helps you address them before they become more pronounced. Here are the key early warning signs:
Visible Red or Purple Lines
The most obvious early sign is the appearance of fine, branching lines on the skin. These typically appear in red, purple, or blue colors and may be clustered in one area or dispersed across a larger region.
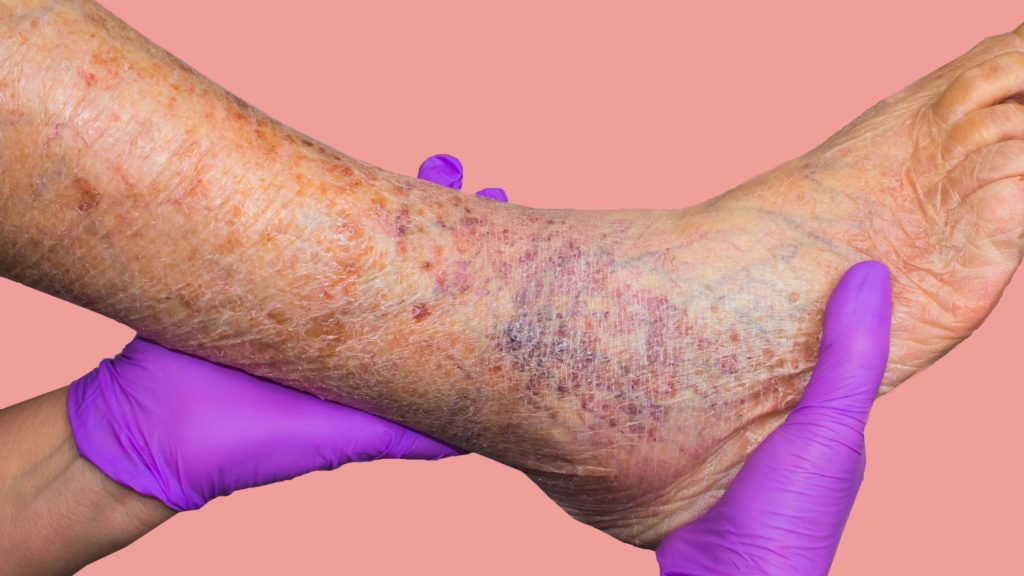
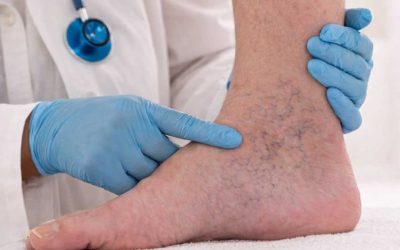
Spider Vein on Ankles and Feet
Spider veins on ankles and feet are among the most common presentations, particularly because these areas experience increased pressure from gravity and standing. The lower extremities bear the weight of your body, making them susceptible to venous dysfunction.
Facial Spider Vein
Facial spider vein development often indicates weakened vessel walls or increased facial capillary fragility. These delicate vessels on the nose, cheeks, or chin can be triggered by sun damage, rosacea, or genetics.
Spider Veins on Nose
Spider veins on nose are particularly visible due to the thin skin and increased capillary density in this area. They may appear as fine red or purple lines and are often associated with rosacea or sun exposure damage.
Mild Discomfort or Heaviness
Although spider veins are typically painless, some people report mild aching, heaviness, or itching in the affected areas, particularly at the end of the day or after prolonged standing.
Pro Tip: If you notice visible veins becoming more pronounced or new ones appearing rapidly, document them with photos. This helps track progression and provides valuable information when consulting a healthcare provider.
What Causes Spider Veins?
Understanding the cause of spider veins is essential for prevention. Multiple factors contribute to their development:
Genetic Predisposition
If your parents or close relatives have spider veins or varicose veins, your risk increases significantly. Genetics influences vein wall elasticity and valve function, making heredity the strongest predictor.
Age and Hormonal Changes
As we age, vein walls naturally weaken. Therefore, women entering menopause face an increased risk due to declining estrogen, which weakens connective tissues supporting blood vessels.
Prolonged Standing or Sitting
Occupations requiring extended standing (nursing, retail, teaching) or sitting (office work, driving) impair blood flow. The reasons include increased venous pressure and reduced muscle pump activity.
Pregnancy
Pregnancy increases blood volume by 40-50% while hormonal changes relax vein walls. Research shows that up to 40% of pregnant women develop spider veins or varicose veins, though many improve after delivery.
Sun Exposure Damage
Chronic sun exposure damages facial skin and weakens capillary walls, especially on the nose and cheeks. This is why facial spider veins are often associated with high UV exposure.
Rosacea and Skin Conditions
Chronic skin inflammation and conditions like rosacea increase facial capillary visibility and fragility.
Obesity and Weight Gain
Excess weight increases venous pressure in the legs, contributing to spider vein and varicose vein development.
Alcohol Consumption
Chronic alcohol use can damage liver function and increase venous pressure, promoting spider vein development.
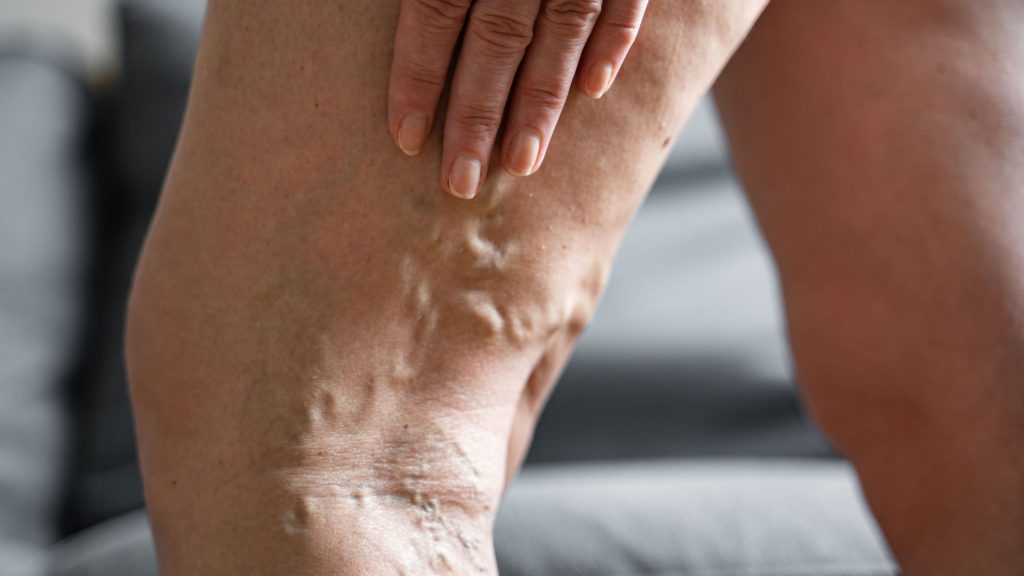
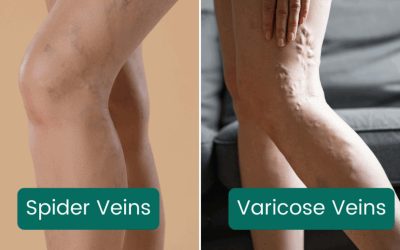
Spider Veins vs. Varicose Veins
Many people confuse spider veins with varicose veins. While they share some causes, they are distinct conditions:
| Characteristic | Spider Veins | Varicose Veins |
| Appearance | Fine, thin, branching lines (red, purple, or blue) | Thick, bulging, twisted veins (dark blue or purple) |
| Size | Less than 1mm in diameter | 3mm or larger in diameter |
| Depth | Superficial (at skin surface) | Deeper (visible under skin) |
| Symptoms | Usually cosmetic only; mild aching possible | Pain, swelling, heaviness, skin changes |
| Medical Risk | Minimal; primarily cosmetic concern | Can lead to blood clots and skin ulcers |
| Valve Function | Usually normal | Faulty valves allow blood backflow |
The dissimilarity between varicose vs spider veins is important because varicose veins pose greater health risks and may require more aggressive treatment. If you’re unsure which type you have, a professional evaluation is recommended.
How to Prevent Spider Veins?
While genetics play a significant role, lifestyle modifications can reduce your risk of developing spider veins or slow their progression. Here’s how to prevent this:
Maintain Healthy Blood Circulation
- Exercise regularly: Aim for 150 minutes of moderate aerobic activity weekly. Walking, swimming, and cycling pump blood back to the heart and prevent pooling.
- Elevate your legs: Spend 15-20 minutes daily with legs elevated above heart level to reduce lower extremity venous pressure.
- Avoid prolonged immobility: If your job requires standing or sitting, take movement breaks every hour.
Protect Your Skin
- Apply sunscreen: Use SPF 30+ daily, especially on the face and neck, to prevent UV damage to capillaries.
- Avoid excessive heat: Saunas, hot baths, and prolonged sun exposure dilate blood vessels.
Dietary and Lifestyle Adjustments
- Improve circulation through diet: Foods rich in flavonoids (berries, citrus) and omega-3 fatty acids support vein health.
- Stay hydrated: Proper hydration maintains optimal blood viscosity and supports circulation.
- Limit alcohol: Excessive alcohol consumption weakens vein walls and increases venous pressure.
- Maintain a healthy weight: Extra weight increases abdominal and leg venous pressure.
Compression and Supportive Measures
- Wear compression socks: Graduated compression (15-20 mmHg) improves venous return and reduces pooling.
- Avoid tight clothing: Restrictive pants or girdles restrict circulation in the legs.
- Choose proper footwear: High heels restrict calf muscle function; vary heel height daily.
Spider Vein Treatment Options
When lifestyle modifications aren’t sufficient, or you prefer cosmetic improvement, several evidence-based treatment options are available.
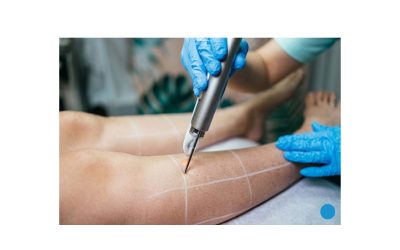
Laser Treatment for Spider Veins
Laser treatment for spider veins is among the most popular professional options. The American Academy of Dermatology recognizes laser therapy as an effective treatment for superficial veins. Intense Pulsed Light (IPL) therapy and Nd: YAG lasers provide options for different vein characteristics.
How it works: The laser emits light energy that targets hemoglobin in the blood vessel. This heat damages the vein wall, causing it to collapse and eventually fade.
Advantages:
- Non-invasive and requires no injections
- Quick treatment sessions (15-30 minutes)
- Minimal downtime; return to normal activities immediately
- Effective for red and purple veins on the face and body
Considerations:
- May require 2-4 sessions for optimal results
- Temporary redness or bruising may occur
- Not ideal for blue veins or very fine lines
- Results typically appear within 4-6 weeks
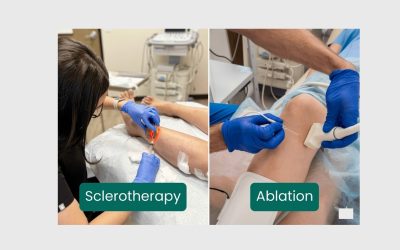
Sclerotherapy for Spider Veins
Sclerotherapy for spider veins is a minimally invasive procedure with decades of clinical success. Medical literature demonstrates sclerotherapy effectiveness rates exceeding 80% for spider vein elimination.
How it works: A tiny needle injects a sclerosing agent (foam or liquid) directly into the vein. The irritant causes the vein wall to collapse, and scar tissue seals it shut, redirecting blood to healthy veins.
Advantages:
- Highly effective for all vein colors and sizes
- Single treatment often produces visible results
- Works well for clustered veins
- Cost-effective compared to laser therapy
Considerations:
- Temporary itching, bruising, or skin discoloration
- Requires compression stockings for 3-7 days post-treatment
- Swelling or temporary darkening of treated veins
- Results appear gradually over 2-4 weeks
Radiofrequency and Other Advanced Treatments
Emerging technologies like radiofrequency ablation and LED-based therapies offer alternatives for patients seeking non-laser solutions.
Treatment Considerations by Location
Spider Veins in Feet and Ankle Veins
Spider veins in feet and ankle veins spider presentations are most common due to gravity and pressure. These areas benefit particularly from compression therapy and elevation, with laser or sclerotherapy offering effective cosmetic solutions.
Spider Veins on Face Treatment
Spider veins on face treatment require specialized approaches due to delicate facial skin and intricate vascular anatomy. Facial spider vein correction often employs gentler laser settings or diluted sclerosing agents. Sun protection becomes paramount for long-term results.
When Should You See a Cardiologist?
While most spider veins are harmless, certain situations warrant professional cardiovascular evaluation. Understanding when to worry about spider vein is essential for your health.
Spider Veins Are Usually Benign
In isolation, spider veins represent a cosmetic concern with minimal medical risk. They don’t cause blood clots, don’t restrict blood flow significantly, and don’t typically progress to serious vascular disease.
Spider Vein and Underlying Venous Disease
While spider veins themselves are superficial, they occasionally coexist with deeper venous insufficiency. In these cases, professional assessment ensures underlying vein function is optimal.
Seek immediate medical attention if you experience:
- Sudden onset of widespread spider veins accompanied by pain or swelling
- Spider veins with signs of infection (warmth, redness, pus)
- Rapid growth or significant darkening of veins
- Associated symptoms like swelling, skin changes, or ulceration
- Family history of blood clots (thrombosis) or deep vein thrombosis (DVT)
Expert Cardiovascular Assessment in Your Community
With over 25 years of experience in cardiovascular and vascular care, Dr. Shalaby, a renowned cardiologist in Webster, provides a comprehensive evaluation of spider veins in the context of overall vascular health. Serving Clear Lake, Webster, Kemah, and surrounding areas, Dr. Shalaby’s expertise at Texas Heart Institute, St. Luke Hospital, Clear Lake Regional Medical Center, Memorial Southeast Hospital, St. John Hospital, and Mainland Medical Center ensures thorough assessment.
A cardiologist in Webster Texas can:
- Evaluate overall cardiovascular and venous health
- Assess for underlying venous insufficiency using ultrasound
- Determine if spider veins indicate the need for deeper vein evaluation
- Coordinate comprehensive care addressing both cosmetic and medical concerns
- Monitor for any progression requiring intervention
The Final Statement
Spider veins are common, usually benign vascular concerns that affect millions. Recognizing early signs—whether on your ankles, feet, face, or nose—allows you to prevent progression and pursue cosmetic improvement when desired.
While spider veins rarely require urgent medical attention, understanding their causes and exploring prevention strategies offers long-term benefits. So, don’t hesitate to seek professional evaluation if you’re uncertain about your vascular health or want personalized treatment guidance.
With specialized experience in cardiovascular and vascular health, Dr. Shalaby, a reputed vascular doctor for varicose veins, provides comprehensive spider vein evaluation and spider vein treatment guidance in Clear Lake, Webster, Kemah, and surrounding areas.
For expert assessment and personalized treatment for varicose veins and spider veins recommendations, call 281-956-7070Or visit The Vein Center at Dr. Shalaby’s website to learn more about spider vein and varicose vein treatment options.